Artificial intelligence’s influence on medical imaging, particularly in ophthalmology, has reached new heights. A pivotal study published in Nature Communications in 2026, led by Zhou, Wang, and Wu, explores the significant role of pre-training data in developing foundation models for analyzing retinal images. Utilizing two extensive fundus image cohorts, the research provides insights that could significantly shape AI applications in eye care worldwide.
Retinal foundation models represent a cutting-edge category of AI tools designed for various ophthalmic applications, including automated disease diagnosis, prognosis, and treatment response prediction. These models undergo “pre-training” on large-scale datasets to acquire generalizable image representations before being fine-tuned for specific tasks. However, the impact of pre-training data on the models’ learned features and clinical applicability has remained an under-explored area. Zhou and his team addressed this knowledge gap by analyzing diverse pre-training scenarios using fundus image data from two distinct cohorts.
The first cohort comprises over 100,000 images collected from a large urban hospital system, showcasing a wide variety of retinal pathologies, image qualities, and patient ethnicities. The second cohort, with nearly 90,000 images from a rural healthcare network, reflects different socioeconomic and clinical contexts. By comparing these datasets, the researchers examined how variations in medical, demographic, and imaging conditions influence model performance.
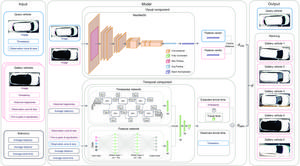
The team’s methodology involved constructing multiple foundation models pre-trained on different subsets of the datasets, ranging from exclusively urban data to fully mixed urban-rural compositions. Utilizing advanced convolutional neural network architectures tailored for high-resolution fundus images, they optimized training protocols to isolate the effects of pre-training data diversity. Subsequent evaluations on independent diagnostic tasks revealed significant differences in performance metrics, particularly in sensitivity and specificity for detecting diabetic retinopathy and glaucoma.
One notable finding indicated that models pre-trained using more heterogeneous datasets—encompassing variations in ethnicity, disease prevalence, and imaging device characteristics—exhibited greater generalizability on external test sets. This finding challenges the conventional practice in AI ophthalmology of relying heavily on narrowly sourced images for pre-training, which poses risks of model bias and diminished applicability among underrepresented patient subgroups. The results suggest that prioritizing data diversity during the pre-training stage not only enhances accuracy but also promotes health equity by reducing disparities in AI-driven diagnoses.
The research team also explored feature representation, using advanced explainability tools to decode what the models learned during pre-training. Models trained on more diverse cohorts displayed richer feature extraction capabilities, capturing subtle retinal texture variations and vascular patterns associated with early disease stages. In contrast, models trained on less diverse datasets tended to overfit superficial image traits, limiting their adaptability and clinical relevance. This underscores the complex relationship between data heterogeneity and the learned internal representations that are essential for effective deep learning models in ophthalmology.
In addressing practical considerations, the research team evaluated computational efficiency and data access constraints that often affect dataset selection for clinical AI projects. By rigorously assessing model training time and convergence relative to dataset size and diversity, they offer actionable guidance for balancing resource demands with model robustness. Their findings advocate for collaborative data-sharing initiatives, particularly across heterogeneous cohorts, to facilitate the development of more reliable retinal AI tools.
The implications of this study extend beyond retinal imaging into broader medical AI fields, where the principles of foundation model pre-training and data provenance warrant further examination. Zhou and his colleagues’ innovative approach illustrates how leveraging large-scale heterogeneous medical datasets can expose latent biases and foster the development of AI models that are both robust and equitable. As the adoption of AI in clinical settings accelerates, these insights are likely to influence regulatory frameworks and best practices for dataset curation and model validation.
Moreover, their investigation into transfer learning paradigms in retinal AI effectively bridges engineering and clinical perspectives by demonstrating how foundational data choices affect downstream diagnostic outcomes. This translational relevance positions the study as a crucial reference for clinicians, AI developers, and healthcare policymakers aiming to leverage AI’s full potential in advancing eye health globally.
While the authors acknowledge limitations in their approach, including the necessity for broader population-level data and prospective clinical validation, the scale and rigor of their research set a new standard in ophthalmic AI. Their findings catalyze future studies focused on refining dataset strategies to optimize foundation models for diverse clinical environments.
In summation, this study redefines our understanding of the critical role pre-training data plays in shaping retinal foundation models. By utilizing two vast and distinct fundus image cohorts, Zhou and colleagues illuminate how data heterogeneity impacts model robustness, fairness, and clinical utility. The findings prompt the AI in ophthalmology community to rethink data collection strategies and emphasize inclusivity in dataset compilation—an essential shift that promises to advance precision eye care globally through intelligent, equitable AI.
As AI-driven retinal diagnostics rapidly evolve, the lessons from this research resonate across broader medical imaging disciplines, striving for truly generalizable and unbiased artificial intelligence systems. Zhou et al.’s work serves as a clarion call to embrace data diversity as a foundational design principle, ultimately empowering AI to better address the needs of millions affected by vision-threatening diseases worldwide.
Subject of Research: The impact of pre-training data composition on the performance and generalizability of retinal foundation models using large-scale fundus image cohorts.
Article Title: Understanding pre-training data effects in retinal foundation models using two large fundus cohorts.
Article References:
Zhou, Y., Wang, Z., Wu, Y. et al. Understanding pre-training data effects in retinal foundation models using two large fundus cohorts. Nat Commun (2026). https://doi.org/10.1038/s41467-026-70077-z
Image Credits: AI Generated
Tags: AI model generalizability in eye care, AI-driven prognosis prediction retina, deep learning in ophthalmology, foundation models for retinal analysis, fundus image dataset impact, medical imaging artificial intelligence, ophthalmic AI applications, pre-training data influence on AI, retinal AI models pre-training effects, retinal disease diagnosis AI, retinal image analysis AI, robustness of retinal neural networks.
See also AI Boosts Research Output by 3x but Reduces Topic Diversity, Study Finds
AI Boosts Research Output by 3x but Reduces Topic Diversity, Study Finds Vertex Group Launches Rs 100 Crore Responsible AI Lab to Boost Ethical AI Development
Vertex Group Launches Rs 100 Crore Responsible AI Lab to Boost Ethical AI Development AI Adoption Reveals Stark Divide: High-Income Countries Use 4x More AI Than Others
AI Adoption Reveals Stark Divide: High-Income Countries Use 4x More AI Than Others LG AI Research Institute Launches Next-Gen VLM ‘Experts 4.5’ for Humanoid Robots
LG AI Research Institute Launches Next-Gen VLM ‘Experts 4.5’ for Humanoid Robots AI Study Reveals Cancer Diagnosis Tools Rely on Hidden Shortcuts, Not True Biology
AI Study Reveals Cancer Diagnosis Tools Rely on Hidden Shortcuts, Not True Biology