A groundbreaking AI-driven cancer testing system could help save lives by showing doctors which drugs are most likely to work before treatment even begins. The technology, developed by the UK-based company PreComb, allows scientists to grow tiny living replicas of a patient’s tumor in the lab and test them against dozens or even hundreds of different drugs and drug combinations to identify the most effective treatment.
Artificial intelligence plays a crucial role in this process, analyzing results at high speed and providing doctors with a clearer understanding of which treatment is most likely to be effective for specific cancers. PreComb is currently focusing on various types of cancer, including small-cell lung cancer, bowel cancer, bone cancer, and brain cancers affecting both adults and children. Experts believe this innovation could significantly improve care for thousands of patients, potentially buying time or even saving lives for those with aggressive tumors.
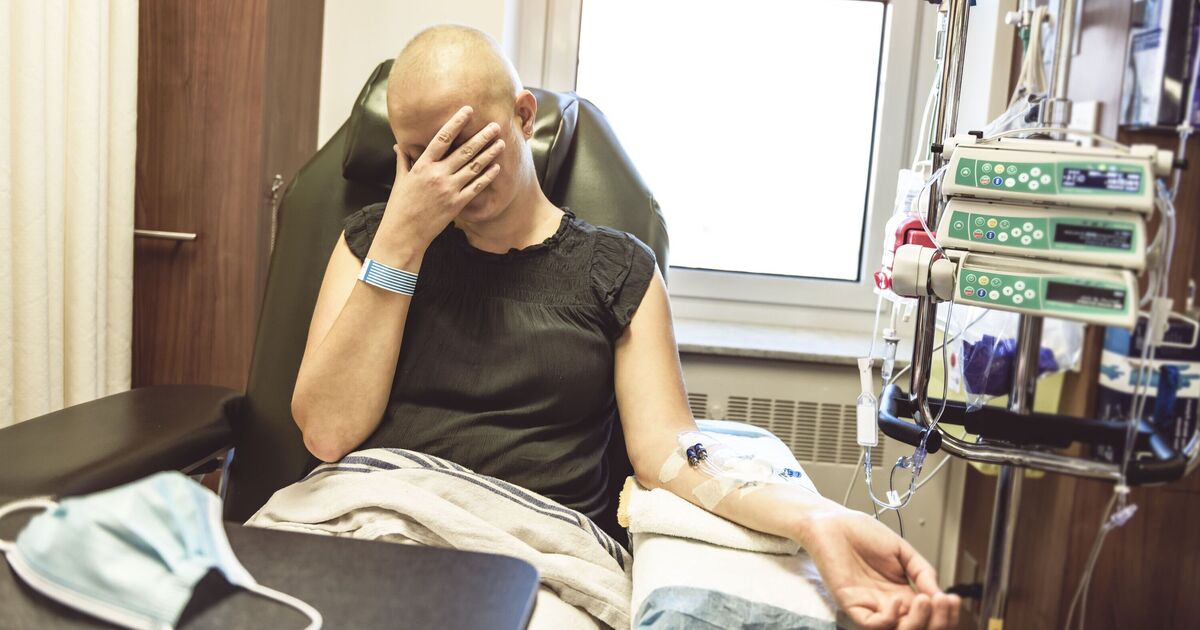
Each year in the UK, around 412,000 people are diagnosed with cancer, equating to one diagnosis every 75 seconds, with over 100,000 patients receiving chemotherapy. Despite its widespread application, chemotherapy drugs are often administered without prior knowledge of their effectiveness for individual patients, largely due to the complexity of cancer itself. Each tumor can behave differently based on its mutations and biology, leading many patients to experience toxic side effects from treatments that do not effectively target their specific cancer.
Scientists are optimistic that this new approach, termed “functional precision oncology,” could change the standard practice. Unlike traditional methods that rely on historical data about average responses in patients, this technique allows researchers to test treatments directly on living tumor material obtained from the patient. Professor Javad Nazarian, an oncology scientist at the University of Zurich, is applying this technology specifically for children with aggressive brain cancers. “These are very deadly tumors and, in many cases, they are still incurable,” he noted.
Until now, doctors have lacked a reliable method to assess how a patient’s cancer responds to different drugs. The new AI-driven drug screening platform enables scientists to test therapies directly on tumor cells sourced from patients. By removing a small piece of tumor tissue, scientists can cultivate living cancer cells, creating a miniature version — or “avatar” — of the patient’s cancer. These mini tumors are then exposed to a wide array of drugs tailored to match the tumor’s genetic profile.
Professor Nazarian’s team can test over 120 drugs that might be effective against a patient’s specific tumor biology. Unlike standard chemotherapy, which indiscriminately targets fast-growing cells, the goal here is to pinpoint treatments that specifically target the tumor. Over a period of two to three weeks, the platform meticulously monitors the tumor cells, with artificial intelligence analyzing thousands of images to determine whether the cells are proliferating, stabilizing, or dying off.
Professor Nazarian stated, “When fully developed, the system will give doctors a far clearer view of what is happening. We can tell if the cells are expanding or falling. The AI platform helps us see whether tumor cells are dying, proliferating, or becoming dominant. That could hugely advance the way we treat patients.” For brain tumors, where clinicians often have limited time after surgery to decide on a treatment plan, the need for speed in analysis could be critical, he added.
He recounted a case where one child, initially expected to survive only three months, lived for 19 months after utilizing the screening approach to guide treatment. “The tumor eventually recurred, but some of it disappeared, extending survival,” he said. The PreComb system employs automated robotics and specialized well plates containing miniatures of the original tumor, enabling a large number of drug tests to be conducted simultaneously. Chief Executive Hal Bosher emphasized the efficiency of the platform, stating it generates approximately 5,500 images per test. With advancements in AI and machine learning, meaningful outcomes can now be extracted from this vast data.
PreComb has completed 371 screens, generating over 1.1 million tumor images across 272 different drugs. As this technology continues to evolve, it holds the promise of transforming cancer treatment protocols, providing personalized therapies that could revolutionize outcomes for patients facing aggressive malignancies.
See also Autoscience Secures $14M Funding to Launch World’s First Automated AI Research Lab
Autoscience Secures $14M Funding to Launch World’s First Automated AI Research Lab OFC 2026 Attracts 18,000 Attendees, Showcases AI Infrastructure Advancements
OFC 2026 Attracts 18,000 Attendees, Showcases AI Infrastructure Advancements AI-Driven Impurity Profiling Enhances Genetic Toxicology Testing, Market to Reach $5.97B by 2035
AI-Driven Impurity Profiling Enhances Genetic Toxicology Testing, Market to Reach $5.97B by 2035 Emily Wright Advocates for Solar Energy Research in Meetings with Georgia Lawmakers
Emily Wright Advocates for Solar Energy Research in Meetings with Georgia Lawmakers Elon Musk and Demis Hassabis Debate AI’s Future in Scientific Discovery on X
Elon Musk and Demis Hassabis Debate AI’s Future in Scientific Discovery on X