A novel blood test, alongside a standardized questionnaire enhanced by artificial intelligence, is poised to revolutionize leprosy diagnostics in Brazil. Researchers from the University of São Paulo (USP) implemented this innovative method using blood samples collected during a COVID-19 population survey, demonstrating its promise in identifying the disease at earlier stages when conventional laboratory tests often prove inadequate.
The study was conducted by the Department of Clinical Medicine, Biochemistry, Immunology, and Social Medicine at the Ribeirão Preto School of Medicine of USP, with support from the São Paulo Research Foundation (FAPESP). Led by researcher Marco Andrey Frade, the findings were published in the journal BMC Infectious Diseases.
“Leprosy is an ancient disease, yet it still faces challenges typical of neglected health issues,” said Filipe Lima, a biomedical scientist and co-author of the study. He noted a significant gap in sensitive laboratory technologies for early diagnosis and a lack of preparedness among healthcare professionals to recognize the disease’s initial stages. This situation is compounded by the fact that standard treatment methods have remained unchanged for over 40 years, leading to treatment failures and bacterial resistance.
To tackle these challenges, researchers focused on identifying new biomarkers and diagnostic tools. Utilizing blood samples from a serological survey conducted during the COVID-19 pandemic, they aimed to pinpoint individuals potentially exposed to the leprosy bacillus and to identify new cases earlier.
Central to the new diagnostic approach are two screening tools. The first is the Leprosy Suspicion Questionnaire (LSQ), comprising 14 questions primarily centered on neurological signs and symptoms. This questionnaire was augmented with an artificial intelligence system dubbed MaLeSQs. The second tool is a blood test that detects antibodies to the Mce1A antigen, which plays a crucial role in the survival of Mycobacterium leprae within human cells. Current tests typically detect the PGL-I antigen, but the anti-Mce1A test analyzes three antibody classes—IgA, IgM, and IgG—enhancing sensitivity and aiding in the distinction between exposure, active infection, and prior contact.
“Unlike the traditional [anti-PGL-I] test that typically identifies antibodies only in severe cases, the Mce1A test enables earlier identification of both contact with the bacillus and active disease,” Lima explained. Traditional tests often yield positive results only in advanced stages of the disease when lesions are already present.
To evaluate their findings, researchers invited approximately 700 participants from the COVID-19 survey to partake in the leprosy study. Out of these, 224 responded positively to the digital questionnaire, and 195 underwent blood analysis. All participants were also encouraged to seek in-person evaluations from specialist physicians, a critical step for confirming diagnoses.
From those who attended the consultations, 12 new leprosy cases were diagnosed, representing nearly one-third of the individuals evaluated. “These are people who had no obvious symptoms and were unaware they were ill, but were diagnosed thanks to our project,” Lima noted. The IgM antibody test for the Mce1A antigen proved most effective, identifying two-thirds of the newly confirmed cases. When combined with the AI tool, the diagnostic approach achieved 100% sensitivity, flagging all suspected cases that were later confirmed during in-person consultations.
“While the blood test alone does not confirm a leprosy diagnosis, it serves as a critical tool for identifying those who require further evaluation by a specialist,” Lima stated. The cost of this new diagnostic approach is similar to existing tests, making it accessible for clinical laboratories. “These techniques are low-cost and straightforward to perform,” he added.
The study also utilized georeferenced maps to analyze the spatial distribution of identified cases, revealing a diffuse pattern of exposure to the bacillus. “This randomness indicates that leprosy is not confined to specific regions but rather is distributed throughout the city among various socioeconomic groups,” Lima explained.
Leprosy is an infectious disease that primarily impacts the skin and peripheral nerves, leading to symptoms such as pale or reddish patches, loss of sensation, and muscle weakness. According to the World Health Organization, over 200,000 new cases are reported annually, mainly in low- and middle-income countries. Brazil ranks second globally in reported cases, trailing only India, and accounts for approximately 90% of cases in the Americas.
The next phase for the researchers involves advancing the validation of these diagnostic tools for broader application within Brazil’s national public health system (SUS). Additionally, Lima is exploring the potential for increasing the specificity of the Mce1A marker by studying smaller regions of the protein to develop an even more sensitive and accurate test.
See also UCLA Study Reveals AI’s ‘Body Gap’ Could Compromise Safety and Trustworthiness
UCLA Study Reveals AI’s ‘Body Gap’ Could Compromise Safety and Trustworthiness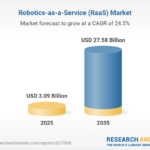 Robotics-as-a-Service Market to Reach $27.58B by 2035, Driven by AI and Automation
Robotics-as-a-Service Market to Reach $27.58B by 2035, Driven by AI and Automation JMIR’s Dr. Chew Calls for Science Publishing Overhaul to Tackle AI Reproducibility Crisis
JMIR’s Dr. Chew Calls for Science Publishing Overhaul to Tackle AI Reproducibility Crisis Illinois State University Signs AI Partnership with South Korea’s Chungnam University
Illinois State University Signs AI Partnership with South Korea’s Chungnam University UNU and Tsinghua University Launch Hub to Drive Ethical AI Governance in China
UNU and Tsinghua University Launch Hub to Drive Ethical AI Governance in China